Interview with Dr. Heiner Steffen
Specialist in internal medicine, pulmonology, allergology, sports medicine, environmental medicine
All Sensors: Thank you very much, Dr Steffen, for taking the time to speak with All Sensors. You are a specialist in internal medicine, pulmonology, allergology, sports medicine and environmental medicine, and you ran your own practice in Landsberg am Lech for 25 years.
How has spirometry developed as a dedicated diagnostic procedure in respiratory medicine, and what role does it play?
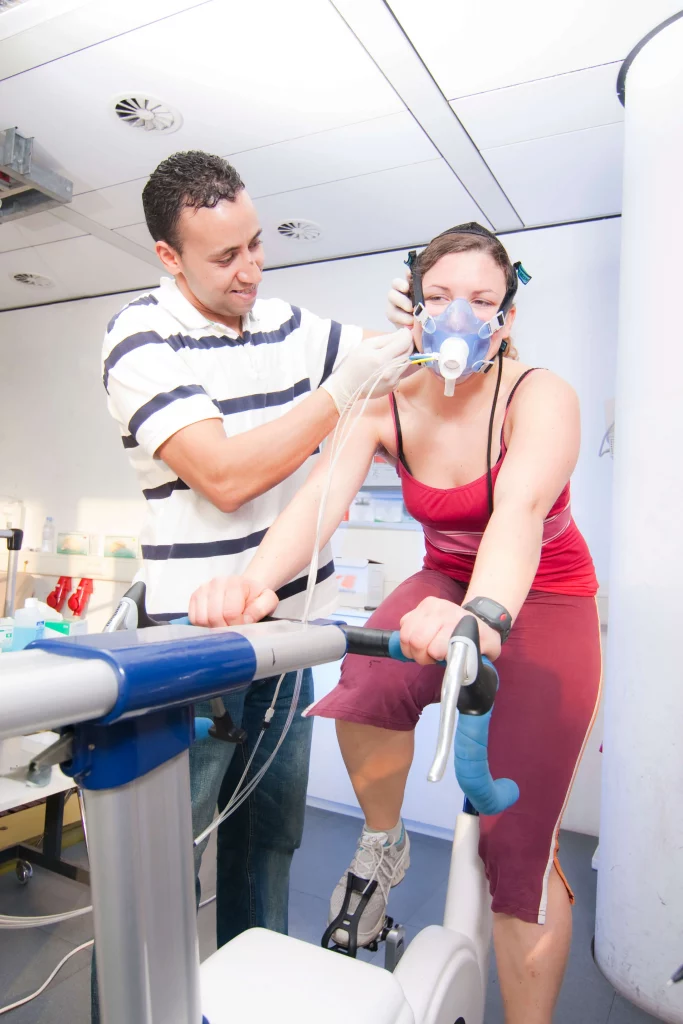
Dr. Steffen: Spirometry is the basic diagnostic method in lung function analysis. It is a simple technique, but it is very much patient-dependent and relies on the interaction between medical staff and the patient. It is an open procedure. Patients wear nose clips so that airflow passes entirely through the mouth, and then a flow-volume curve is recorded. This flow-volume curve provides an immediate visual diagnostic impression, allowing us to assess straight away whether the patient is healthy or unwell and which possible disease patterns may be present.
The flow-volume curve rises steeply and always has a peak, even in cases of restriction or fibrosis. If there is no peak, there is an error somewhere. The volumes should always form a closed curve.
Dr. Steffen: The flow-volume curve shows the patient’s inspiratory capacity and dynamic parameters in terms of expiration, but also forced inspiratory capacity. This is where the dynamic element comes in, because the patient is asked to perform actively.
With body plethysmography, I have an enclosed chamber, which gives me static volume parameters, intrathoracic values and the overall resistance, in other words airway resistance. This procedure takes place without dynamic patient activity.
"Reliability across the long term is the most important factor."
All Sensors: What other parameters are measured in spirometry?
Dr. Steffen: Humidity, temperature and ambient air pressure. These values are needed to correct for the influence of the body’s BTPS conditions. In the early days, we still had to enter these parameters manually into the first body plethysmographs. You had to read them from a hygrometer and thermometer and then enter them into the computer. And when temperatures changed over the course of the day, the process had to be repeated. Here, sensor technology helps to automate the process and reduce the burden on staff.
All Sensors: Would it also be useful to package sensors into even smaller housings, meaning further miniaturisation, or to integrate several sensors into one housing?
Dr. Steffen: Devices that patients take home should be compact and easy to handle while maintaining high reliability. Devices for sleep apnoea diagnostics and for diagnosing obstructive airway disease (COPD) record parameters at home over days and weeks so that the data can then be evaluated centrally. Small sensors are a very good answer here.
All Sensors: How often do spirometers need to be cleaned or calibrated?
Dr. Steffen: Every day we check whether the volume we specify — 3 litres, using a calibrated pump — produces the corresponding curve. Cleaning is also carried out every day. Filters are individualised, then either discarded or given to the patient to bring back for the next visit. Filters are placed upstream of the sensor system to protect it from moisture and contamination.
Intelligent temperature compensation in the sensor system is also important. In practice rooms, the body plethysmograph is exposed to temperature fluctuations over the course of the day due to sunlight and shading, and these must be compensated for. Temperature-based calibration has to be very precise. That saves staff from having to recalibrate the zero curve manually all the time, makes the device easier to use and prevents user errors.

All Sensors: How long is the service life of these devices?
Dr. Steffen: Decades. In practice, you only replace a body plethysmograph when you move premises or when the device becomes old and wear becomes too great, for example if sealing rings start causing faults too often and have to be replaced. We may have bought three or four body chambers, and we always had two in two different rooms.
That is why the reproducibility and long-term stability of the sensors over a period of 10, 15 or 20 years are very important.
All Sensors: To what extent do you currently see changes in diagnostics due to AI? Can AI support the evaluation process, for example?
Dr. Steffen: Evaluation would be something like a diagnostic suggestion, as we already have with ECGs. I think it is helpful when the doctor receives support with interpretation or a hint and suggestion. But the doctor should of course still remain in charge of the ECG printout or the graphical representation of the flow-volume curve.
AI could also help with the measurement itself. For example, in identifying which measurement is poor, or where the patient shows volume fluctuations during inhalation and exhalation. If the algorithm helps to select the measurements with the best quality, AI can support medical staff and improve the process. Especially when evaluating measurements within narrowly defined limits, one can expect better results from AI than from humans.
The future of AI lies in ease of use and in helping to shape interpretation. Spirometric measurement is physics, and that will not change.
“Only comparable measurements over a longer period can form the basis of my treatment decisions”

Dr. Steffen: Yes. In respiratory specialist examinations, both are used. That means the door of the body plethysmograph is open first, and the patient performs the dynamic parameters of the flow-volume curve. That already allows us to estimate what kind of breathing dynamics we can expect. If someone is severely hyperinflated and emphysematous, breathing dynamics are significantly more difficult for them than, for example, for an athletic person.
Then there are specific breathing manoeuvres that are performed in the closed chamber in order to record two additional parameters: intrathoracic gas volume and resistance, meaning airway resistance.
All Sensors: Which are the most important measured values in lung function diagnostics?
Dr. Steffen: On the one hand, the flow-volume curve deals with inspiratory capacity, which can also be measured in a forced, that is dynamic, way. On the other hand, it deals with expiration, peak expiratory flow, or PEF, and the one-second value, FEV1, the major parameter for airway narrowing and airway obstruction. There are also some calculated values derived from these. These are also used to grade disease severity, for example in chronic obstructive airway disease.
All Sensors: What role do pressure sensors play in the measurement? What requirements must they meet?
Dr. Steffen: The sensor system has to respond quickly and be reproducible. That means when the patient is asked to produce the same manoeuvre three or four times, the measurement technology must of course be able to measure the same result reliably and repeatedly. In practice, variability on the patient side is usually much greater. The real question is whether the patient blows properly into the spirometer, inhales fully beforehand and does so reproducibly.
The sensor system generally measures so well that the doctor does not question the measurement technology. In most cases, errors are caused either by the patient or by the staff. However, these can be recognised in the flow-volume curve. There are checking criteria, a kind of visual diagnosis. You can see whether the patient coughed and whether they inhaled sufficiently to exhale the volume they should have produced. Measurement technology is helpful in identifying patient errors such as coughing, throat clearing or inconsistent exhalation. It also gives medical staff confidence in the validity of the measurements and helps to identify results influenced by interfering factors. For this, intelligent sensor technology is needed that measures with sufficient precision.
Experienced specialists can recognise which measurements were unsuccessful and may, for example, take only the average of the best three out of five measurements. Consistency in measurement and reliability of measurement are what matter most. That is more important than the final percentage point of measurement accuracy. In medicine, we are dealing with fundamental decisions: healthy, ill or on the way to becoming ill. In that respect, measurement technology is much more precise than the accuracy of our diagnosis.
All Sensors: Which sensor characteristics, such as response time, accuracy and long-term stability, are the most important, and what improvements or developments would you like to see?
Dr. Steffen: I believe reliability in cross-sectional examinations is extremely important. If the patient comes in today and then returns in a few months or in a year, the same level of reliability in diagnostic quality has to be guaranteed. The same applies when I change a therapy and the patient comes back to the practice repeatedly. I expect my measurements to remain comparable over a longer period. Only then can they form the basis of my treatment decisions. Whether the device measures one millilitre more or less does not have much influence on the decision about whether and how I treat the patient. Long-term reliability across cross-sectional examinations is the most important factor. And the less the doctor has to think about the measurement technology, the more reliable and stable the system is likely to be.
The other important point is the fast sensor response. Especially in dynamic processes, it is important not to lose any decisive information.
All Sensors: In your many years of practical experience, how often have you encountered situations in which the spirometer or body plethysmograph no longer worked reliably?
Dr. Steffen: From time to time. Often there are mechanical causes. For example, a damaged sealing ring can cause leaks. A blocked tube or condensing moisture can also cause errors in volume measurement in the chamber during automatic calibration.
For the doctor, the source of the error is not easy to identify. We can only describe the problem to the technician: the device is not measuring, it has drift, the curve is not returning to its zero line. But we do not know the cause and then need technical support. In most cases, however, these are not sensor issues.
All Sensors: Do you see any further AI developments?
Dr. Steffen: AI could help reduce the diagnostic workload through ever smarter combinations and interpretation of different measured parameters. Therapy would then increasingly take place at home using mobile devices given to patients. This would reduce doctor visits and lower healthcare costs.
All Sensors: Thank you very much for the interview, Dr Steffen.
